Ayurveda Concepts of Asthi Majja kshaya.
“Dosa dhatu mala mulam hi sariram.” Ch sutra, with this concise sloka from the Charaka Samhita (c. 200 BC), Ayurveda reveals the healthy human body as the dynamically balanced state of dosha, dhatu and mala (bioenergies, tissues and wastes). This same point is further elaborated on by Acharya Sushruta a century later with his famous definition of health as Samdosha samagnishch samdhatu malakriya| Prasannatmaindriya manah swastha itibhidhiyate|| “the equilibrium of dosha, dhatu, mala, agni, kriya and prasannata (serenity, clarity) of atma, indriya and manas”. As the Astanga Samgraha (c. 500 AD) further declares: “Shareeram dharayenthe dhatvaharashcha sarvada” meaning the support of the human body is accomplished by entirely dhatu and ahara (tissues and food). “Preenanam Jivanam Lepa Shneho dharan purine | Garbhodpadashch dhatunaam|| Ashtang hrudya 1, among the sapta dhatus (seven tissues), the ashti dhathu (bone tissue) is the one which is bestowed with the supreme function of shareera dharana (bodily support). Asthi dhatu confers structure to the body and protects the vital organs. A human being without asthi dhatu would be a formless blob of soft tissues. Thus, Asthi dhatu can accurately be viewed as the scaffolding by which humankind stands upright and noble. Any discord in the equilibrium of the doshas and dhatus leads to disease.
Asthi Dhatu formation starts in the intra-uterine life. It keeps growing and get nourished by the food just like any other Dhatu.
Asthivahanam strotasam medomoolam jaghanam ch || Precursor of AsthiDhatu (Poshak Asthi) is formed at the time of formation of Medo Dhatu. Nutrients of Asthi Dhatu (Poshak Asthi) reaches the Asthivaha Srotas where it is acted upon, by Asthidhatwagni and results in formation of Poshya Asthi Dhatu,
Asthi-Mala (Kesh, Loma, & Shmashru), Updhatu (Danta) and the formation of Poshak Majja Dhatu.
Asthi Panchbhautikatva Aakash- porous cavity inside bone, Vayu- flow of blood, nutrients etc, Agni- conversion of cartilage into bone, Jala- bone marrow, Prithivi- constitution of bone.
Asthi Dhara Kala:- Purishadhara-Kala is also called the Asthidhara Kala. Purish Vikriti and Agni Vikriti for e.g. Malavishtabha, Grahani etc. are relatively common in Kati-Shula, Sandhi-Shula and Asthi-Shula and it is seen that the treatment of Purish Vikriti also decreases the intensity of such Shula. If Asthidhara-Kala is Purishdhara-Kala as Dalhan suggests, this in between Sleshmadhara and Pittadhara or Majjadhara-Kala. Hence Asthi is between two unctuous Dhatu and two unctuous-Kala as well.
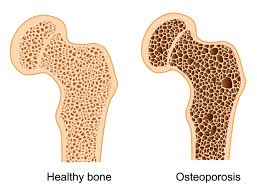
Osteoporosis in Ayurveda
Osteoporosis corresponds most closely to the condition known in Ayurveda as Asthi-majja kshaya. In our classical text books Asthi-majja kshaya is not actually named as a separate disease entity, but rather as one of several consequences which can emerge as a result of Dhatu-kshaya (diminution of tissue). Asthisaushirya, meaning “porous bones,” is another condition not mentioned as a separate condition but as a symptom of Majjakshaya. In addition to being the well-known source of the functionally important haemopoietin tissues, majja dhatu also represents the collagen, fat and protein within the bones which provide strength and stability to the body structure. The Charaka Samhita, Sutrasthana, Chapter 17 describes eighteen types of dhatu-kshaya. It is here that we first see a description which closely resembles our modern-day disease called osteoporosis. The signs and symptoms of this condition are described later in several other all the texts of Ayurveda: thinness, brittleness and lightness of the bones. In addition, other accompanying signs are described: looseness of joints, hair loss from body and beard, tooth weakness, and unhealthy nails.
The samprapti involves vata prakopa (spread) in both the large intestine and asthi dhatu and sthanasamsraya (relocation) to majja dhatu. Asthi dhatu is formed from the posaka (“providing nourishment”) part of meda dhatu (fat tissue) in the purisha dhara kala, situated in the pakwashaya (large intestines), where it is transformed to asthi dhatu by asthiagni. Similarly, Majja dhatu is formed from posaka fraction of the asthi dhatu as it flows through the majjavaha srota and is acted on by the majjagni. The health of Majja dhatu depends on the state of the majjagni. But in asthi-kshaya, Vata increase infiltrates majja dhara kala and majjagni becomes distorted and irregular. This causes majja dhatu (marrow tissue) to be of inferior quality and quantity.
Also, its pathology is eloquently understood by the concept of ashraya-ashrayi bhava—a very important and impressive theory given by Vagbhata in the text Astanga Hridaya. This is a theory which describes the relationship between Dosha and Dhatu. Here is what is said:
Ashraya :- Ashraya means a resting place and that on which anything depends. Ashrayi :- Ashrayi means resting with and depends on. Ashraya and Ashrayi are interdependent. In this- Ashraya is “Receptacle” and the meaning of Ashrayi is “Resorting”. According to this the Vriddhi of Dosha is reflected as Vriddhi of Dushya, and the Kshaya of Dosha in reflected as Kshaya of Dushya. This law is applicable to sleshma (kapha dosha) and pitta dosha, but not in Vata dosha. Ashraya-Ashrayi relationship is helpful to understand the disequilibrium of Dhatus and Malas.
Vata resides in Asthi (bones); Pitta resides in Rakta (blood) and Sweda (sweat); Kapha resides in rest of the Dhatus (tissues) and Mala (waste products).
In case of Pitta and Kapha, when there is an increase of Pitta or Kapha, there is also a corresponding increase of tissues and waste products associated with them. For example, if Pitta increases, then sweat and blood also increase. The same rule applies to decrease as well. But in case of Vata and Asthi it is exactly opposite: if Vata increases, then Asthi decreases and vice versa. They are inversely related to each other. (AH Su 26-27). In the disease process the Ashrayi affects the Ashraya either Dravyataha, Gunataha or Karmataha. By understanding this mutual relationship we can infer the relative changes in the Dosha and Dushya by observing the changes occurring in them. Any change in any of them will reflect on another in the same fashion except in Asthi and Vata. ‘Asthi Marutayoho Na Evam…’ i.e. Vata and Asthi are inversely proportional. Example for Vata: Vataja Aahara Vihara which leads to Vata Dosha Vriddhi which in turn increases the Vayu Mahabhoota present in the Asthi leading to Asthi Kshaya
Causes (Nidana) of Osteoporosis
For any disease, the causative factors described in Ayurveda can be classified into four groups:
- Ahartmaka Nidana (Dietary) 2. Viharatmaka Nidana (Lifestyle Regimens) 3. Manas Nidana (Psychological) 4. Anya Nidana (Other)
With respect to Asthi-Majjaksaya (osteoporosis) here are the classically observed causes:
Ahartmaka Nidana (Dietary)
Aptarpana (lack of nourishing food); Alpashana (inadequate quantity of food); Excessive consumption of Laghu, Katu ahara (light, spicy foods); Ruksha (excessively dry food without oil/ghee);
Viharatmaka Nidana (Lifestyle Regimen)
Ativyayama (excessive aerobic exercise; lack of weight bearing exercise);Vishamadupchara (faulty treatment); Asriksraava (excessive bleeding); Ati Adhva gamana (excessive walking or jogging); Vega Vidharana (control natural urges).
Manshika Nidana (Psychological)
Chinta (stress, tension); Shoka (sadness); Krodha (anger); Bhaya (fear)
Others: Chirkalaj roga (any chronic illness), Aghata (trauma)
Ayurvedic Treatment of Asthi-Majja Kshaya (Osteoporosis)
In Ayurveda, management of any disorder is divided into essential three parts:
- Nidana parivarjana (Removal of the cause(s) 2. Samshodhana (Strong purifying therapies) 3. Samshamana (Gentle, balancing therapies)
Nidana parivarjana. Removal of the cause(s). This is the first line of treatment of any disease and it is most important line of treatment for Asthi kshaya also. Ayurveda says that nidana, the root of the samprapti process (samprapti=developmental stages of disease), must be avoided for best management of the disease. In osteoporosis the factors, i.e., Ahartamaka, Viharatmaka, manas and others which are responsible for the causation of the diseases should be avoided (see above section on “Causes of Osteoporosis.”)
Samshodhana therapy. In short, this refers to a profound biopurification or cleansing of the tissues. Shodhana therapies are procedures by which the aggravated doshas or the accumulated improperly digested products of digestion in the tissues are eliminated after loosening and mobilizing them from their respective sites. Panchakarma is the principal and most effective method for Samshodhana therapy and is recommended at the commencement of treatment and then once or twice each year. I have extensively reviewed Panchakarma procedures in other articles and book chapters so will not elaborate here except to mention the supreme importance of basti karma (therapeutic enemata) and that Tikta Basti (decoctions of bitter-tasting plants) is indicated in osteoporosis. The duration of basti therapy is dependent on rogi- and rogapariksha features (qualities of the patient and the disease) and can be:
- Karma vasti — total of 30 enemas: 6 oil-based then 24 alternating decoction-based and oil-based enemas
- Kala vasti — total of 16 enemas: 6 decoction-based and 10 oil-based 3. Yoga vasti — total of 8 enemas: 2 oil-based then 6 alternating decoction-based and oil-based enemas
Samshamana therapy. These are gentler therapies. Among the upakrama, meaning “frequent rituals” (six types of ritual therapies- snehana, swedana, rukshana, langhana, stambhana, brihana), snehana (oil application) and swedana (fomentation) can be administered for shaman purpose in asthi-khaya. In fact any activity, food, medicine, or thought which possess vata shamaka (vata-pacifying) properties is considered as an ideal for samshamana therapy.
Ayurveda advises the avoidance of the following apathy dietary articles: bitter, pungent, astringent taste dominant substances; dry, cold, light, and excessively spicy predominant substances; Shushkamamsa (dry meat); Shushkashaka (dry vegetables); Madya (alcohol); excessive eating; fasting; heavy exercise; excessive sexual intercourse; day sleep; night awakening; suppression of natural urges. Avoid medicines corticosteroids, anticonvulsant, and other medications known to decrease bone strength; avoid smoking and all other etiological factors which cause aggravation of Vata.
Traditionally used medicines for Asthi-majja khaya (osteoporosis): Single drugs: Asthi shrinkhala ghrita, Shatavari, Ashwagandha churna, Shuddha guggulu, Mukta pisti, Praval pisti, Shankhabhama. Compound drugs: Yograj guggulu, Rasayana churna, Triphala guggulu, Laxadi guggulu, and many others.
In chikitsa medicines which increase or decrease the Ashrayi also increase or decrease respective Ashraya except in Asthi and Vata. E.g.:- Vata aggravates by Ruksha, Tikta, Katu, Kashaya, Apatarpana, Langhana but the same factors decreases Asthi. Vata pacifies by Snigdha, Madhura, Amla, Lavana, Brhmana but these factors contribute to Asthi Dhatu. As Pitta-Rakta and Kapha-Rasa, Mamsadi Dhatu are directly proportional those medications or Dravyas which increase or decrease the one will also increase or decrease the other hence treatment should be planned accordingly.
Morden Treatment Modalities:-
Modern drug therapies for osteoporosis include bisphosphonates, such as alendronate (Fosamax) and risedronate (Actonel) and selective estrogen receptor modulators (SERMs) like raloxifene (Evista). These drugs are associated with a growing list of concerns, including research that suggests a link between the use of bisphosphonates and esophageal cancer. A once-per-month tablet, ibandronate sodium (Boniva), claims the advantage of greater convenience but still has a host of adverse effects, such as back pain, esophageal irritation, heartburn, and ulcers.
Hormone replacement therapy (HRT) was previously promoted as a treatment for osteoporosis, and may, in fact, be somewhat useful for decreasing bone loss. However, this benefit stops if hormone therapy is discontinued. In addition, many women refuse hormone therapy due to other known or perceived adverse effects.
If you are willing to endure the risks and adverse effects of the above mentioned pharmaceutical agents they can be effective. But since the non-pharmacological prevention and treatment of osteoporosis is possible, we can be proactive against this disease through the purification/rejuvenation Panchakarma procedures of Ayurveda, intelligent personalized nutrition, an increase in weight-bearing exercise training, and judicious use of time-tested Ayurvedic herbal medicines. Ayurvedic medicine recognizes the importance of a whole-food diet that includes naturally occurring bone-nourishing elements (i.e., calcium, magnesium, vitamin D, boron, strontium, vitamin K, etc) but does not recommend the use of supplements.
Effective Dietary Interventions
The best approach to getting sufficient nutrients to build and maintain strong bones is to consistently make healthy, organic, whole food choices according to your Prakriti (constitution) and the seasons, however it should be modified in almost all cases towards Vata-pacifying foods. Your diet, and not supplements, is the ideal source for all the bone-specific nutrients mentioned below.
Calcium
Calcium is the most abundant mineral in the human body. It is well recognized for its importance in the development of bones and teeth, in the function of muscles, and has many other functions as well. The common wisdom is that 1,000–1,200 mg/day of calcium is required (varies with age, weight, sex, etc.).
Magnesium
Magnesium is important for more than 300 important metabolic processes, including building bone, forming adenosine triphosphate, maintaining normal nerve and muscle function, and absorbing calcium. Adults need about 300-400 mg per day. Dietary sources of magnesium include nuts, whole grains, dark green vegetables, avocado, banana, soy, fish, meat, and legumes. Magnesium deficiency has been associated with bone loss in several studies.
Vitamin D
Vitamin D is essential for the formation and maintenance of bone tissue, through its regulation of calcium and phosphorous absorption from the intestines into the bloodstream and numerous other metabolic effects. Vitamin D increases the number and activity of osteoblasts, reduces the activity of osteoclasts, and normalizes the turnover of bone. It also helps prevent an over-secretion of parathyroid hormone (PTH) which can activate osteoclasts to increase bone reabsorption, contributing to osteoporosis.
Vitamin D is synthesized when sunlight is absorbed by the skin and transforms 7-dehydrocholesterol into vitamin D3 (cholecalciferol). D3 is shuttled to the liver where it is converted to 25-hydroxycholecalciferol, which is then transformed into 1,25-dihydroxycholecalciferol (calcitriol). Calcitriol is 10 times more potent than vitamin D3. Magnesium and boron act as cofactors in this reaction. Food sources of vitamin D include fish and fish oils. Dietary vitamin D appears to be most effective as a therapy for osteoporosis when combined with dietary calcium.
Dietary Vitamin D has no adverse effects, however Vitamin D supplements can cause intoxication if taken higher doses long-term. Symptoms include weakness, nausea, vomiting, and poor appetite. Toxicity may be seen when serum vitamin D concentration is consistently >200 ng/ml.
Vitamin K
Vitamin K is a fat-soluble vitamin known for its effect in blood clotting, which it partly accomplishes due to its ability to bind calcium ions (Ca2+). Despite being fat-soluble the body does not store significant amounts of vitamin K and it needs replenishment through dietary intake (don’t worry—its widely available) and production by our innate colonic bacteria. Fortunately, vitamin K is to a great extent recycled, which means that even the small amount that is present can be used by the body many times.
Food Sources And Recommendations For Strengthening Bones
Pumpkin seeds, quinoa, millet, brown rice, whole wheat, Swiss chard, artichoke hearts, cashews, tempeh, sweet potatoes, beans, sesame seeds, flaxseed, and wheat germ. Sesame seeds provide 1,000 mg of natural calcium.
Tea: Dandelion tea increases bone density and is quite delicious.
Sleep: Get more sleep. Adults need seven to eight hours of sleep to awaken refreshed.
A study published in 2015 in the Journal of the American Geriatrics Society found that men and women over age 50 who habitually slept less than six hours a night had a substantially increased risk of osteoporosis.
Exercise: Exercise moderately. Exercise may decrease fracture risk by improving bone mass in premenopausal women and helping to maintain bone density in women after menopause. Most experts recommend exercising for at least 30 minutes three times per week.
Yoga: Practice yogasanas such as… single and double leg raises, side angle pose (Parsvakonasana), warrior pose II (Virabhadrasana II), wind relieving pose (Pavanamuktasana), cobra pose (Bhujangasana), seated forward bend (Paschimottanasana), eagle pose (Garudhasana), Locust Pose (Salabhasana), hero pose (Virasana), pose dedicated to the sage Marichi III (Marichyasana III), child’s pose (Balasana), corpse pose (Shavasana).
Bone physiology and bone strength are very complex issues that have important unique nuances in every unique individual. Owing to several unique features of asthi-majja kshaya, Ayurveda considers it curable but only with difficulty (Yapya). These features include: Gambhira Dhatu (bone and marrow are deep-seated tissues), Svabhava Balapravritta Vyadhi(it is a natural phenomenon due to old age) and Bhedawastha(if not prevented in early life it easily reaches the complicated stage of pathogenesis). Management of established loss of bone strength is difficult—but possible by comprehensive intervention as outlined above. Obviously, prevention of the condition through intelligent diet and lifestyle is vitally important and should be commenced early.
<a href=”https://www.teacheron.com/tutor/4E1m?r=4E1m” target=”_blank” style=”display: inline-block;”><img

